Southeast Michigan will need more geriatricians and primary care doctors as the region’s senior population swells, and local health systems are hiring more nurse practitioners and physician assistants to help fill the gap.
Metro Detroit’s population 65 years and older is projected to grow by nearly 148,000 from 2020 to 2030, or 22%, while the region’s population as a whole is only expected to increase by 1% over that period, according to the Southeast Michigan Council of Governments.

At the same time, the state is facing a primary care shortage. Michigan was short 455 primary care doctors in 2023, according to projections by the Robert Graham Center, a Washington, D.C.-based health care policy research firm.
The primary care shortage is felt more acutely with older patients, because they are the ones needing most of the health care, said Dr. Christopher Steffes, an associate dean at Wayne State University School of Medicine. He said seniors often take many medications, and a primary care doctor keeps track of them.
“We’ve got lots of drugs, but somebody’s got to be in charge of which ones are best and for each individual patient based on age and physiology,” Steffes said.
Experts say other medical specialties critical to seniors are also facing shortages.
Dr. Daniel Carey, president of Corewell Health William Beaumont University Hospital in Royal Oak, said geriatrics and palliative care are in particular demand by the aging population. Geriatrics is a field that addresses patients’ geriatric syndromes, such as dementia and falls. Palliative care focuses on symptom relief, pain control and aging in place despite chronic conditions, Carey said.
Some health systems are planning to add more doctors to their workforce. Henry Ford Health will be adding more than 25 primary care providers in 2026, said Dr. Jerry Finkel, the system’s chief primary health officer. Henry Ford Health and Corewell Health are hiring more physician assistants and nurse practitioners. These professionals, called advanced practice providers, can help make up for the lack of primary care doctors, and some of them are trained in geriatrics or palliative care.
As the region’s population ages, Henry Ford Health is also trying to move care “upstream” to keep patients healthy, Finkel said. The health system wants at-risk patients to visit the doctor more often, so they won’t end up in the emergency room.
“When we say move care upstream, what we really mean is changing the way that you think about delivering care from what has traditionally been very reactive ― whoever shows up in my office; this is my priority ― to prioritizing then patients that we’re being very proactive with,” he said.
He said Henry Ford is using technological tools to determine which patients will need “the most care moving forward,” and it proactively reaches out to them.
Meanwhile, Corewell Health William Beaumont University Hospital has six full-time geriatricians, but there’s demand for 12 of those practitioners, said Carey, the hospital’s president.
“You cannot really have enough geriatrician(s) to take care of all the elderly population,” said Dr. Khaled Imam, director of geriatric medicine at the hospital.
So Corewell Health needs to give other doctors, including those in internal medicine and family medicine, “enough knowledge and skills in geriatric medicine to take care of the elderly population in a proper way,” he said.
Imam said some emergency medicine physicians at Corewell received training in geriatric medicine after completing their residency.
Geriatricians play an important role
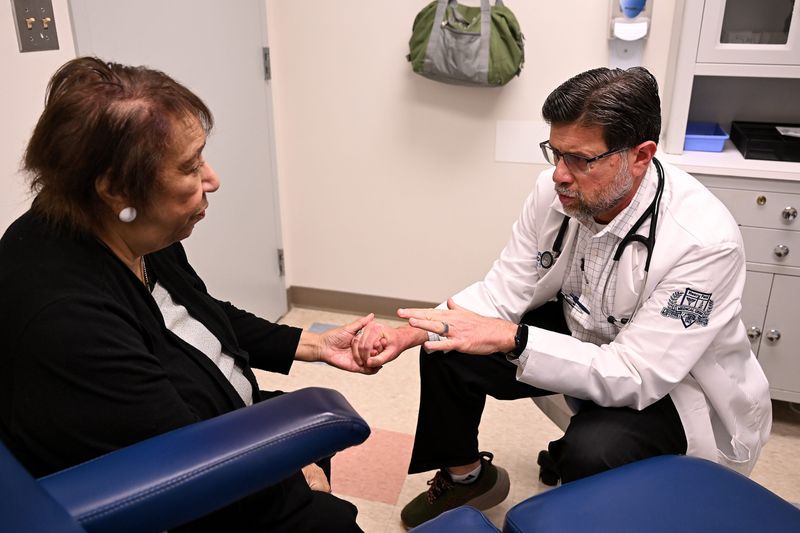
Detroit resident Althea Anderson went to see her primary care physician, Dr. Mirza Beg, a few days after passing out at a restaurant.
During an appointment with Beg, a geriatrician, on Oct. 14 at Henry Ford Medical Center-Livonia, he asked her specific questions about the episode. He asked if she was with her friend, who is a nurse. She said yes.
“Were you done with your lunch, or were you still working on it?” he then asked.
“I was finished with my lunch, pretty much,” Anderson responded, “and I was just sitting there, and all of a sudden, I knew what was coming, because the light starts like this, and then it gets like 3D, and it’s just like sunshine, like bright sunshine. And I just knew that I was going to pass out. I looked at her, told her, and she kept me from falling on the floor.”
She was taken to William Beaumont University Hospital in Royal Oak. Beg said the health workers did a thorough work-up on her. The tests came back negative, except for her blood-sugar levels, which were high.
Beg, division head of geriatrics at Henry Ford Health, said specialized geriatric clinics like his give patients an opportunity to address issues specific to age. Geriatricians give attention to the patient’s memory, gait, balance and nutritional status.
They focus on the patient’s overall well being, instead of “just focusing on hypertension or diabetes or congestive heart failure,” Beg said.
“We have to address those things too, along with their other geriatric syndromes, because, you know, my philosophy is: you are managing a person as a whole” and not just a disease or a diagnosis, Beg said.
He said that geriatricians do a one- or two-year fellowship after finishing a residency in internal or family medicine.
Beg said not many people are going into geriatrics because “it’s challenging.” He said the majority of people who enter the field have a lot of interest in it, because “there’s no really financial benefit as a geriatrician.” The average annual compensation in geriatrics is $289,201, the 13th lowest compensation of 50 medical specialties, according to a 2024 report by Doximity.
Later during Anderson’s appointment with Beg, he said her fainting could be due to postprandial hypotension, which is a drop in blood pressure after eating. The condition is relatively common in older patients, he later told The News.
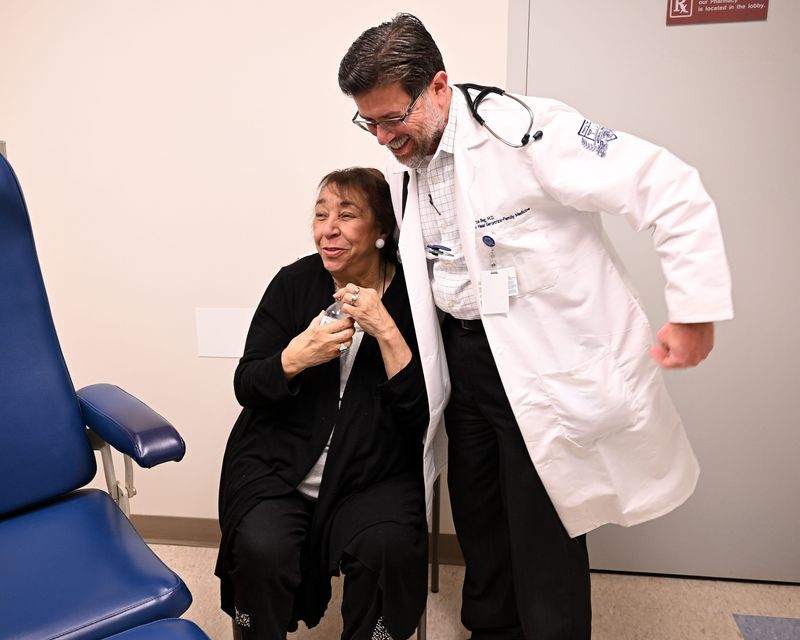
He tweaked Anderson’s medication dosages, including for Lasix, a water pill. Beg, who Anderson said has been her doctor for around 20 years, held her hand while talking to her at the end of the appointment. He said another worker at the doctor’s office would be giving her paperwork, and he had put instructions for her on it.
They ended the meeting with a hug.
Medical schools try to spark students’ interest
To help address the shortage of physicians, Metro Detroit’s two medical schools are encouraging their students to consider careers in primary care.
Finkel, of Henry Ford Health, said that family medicine residencies are “really the key” to the future of primary care. But family medicine has a higher percentage of unfilled positions during Match Day, which is when graduating medical students are matched with a residency program, each year, than other specialties. Henry Ford’s family medicine residencies fill, though, Finkel said.
“There’s not as much interest in being a primary care physician,” he said. “It’s a hard job. It requires long hours, and it requires a breadth of knowledge that is broader and wider than most.”
He said there’s a need for more primary care doctors for all ages of patients, but the senior population requires more time. He said doctors sometimes will have extended visits with seniors.
Steffes, the associate dean of clinical education at Wayne State’s medical school, said his school has efforts to get more of its students interested in primary care.
He said Wayne State is piloting a program to expose first-year students to primary care. The school brings in primary care physicians to help teach its first-year class. The doctors tell the students how they use anatomy, biochemistry and other subjects to take care of patients.
In students’ second year, they spend half a day at a primary care doctor’s office every two weeks. In their fourth year, students can choose to do a rotation, or spend a month, with a geriatrician.
These efforts are meant to get students interested in geriatrics or serving older adults.
“If you’re exposed to it, you’re more likely to say, ‘Wow, I really like old people,’ and I do. … I love my patients,” said Steffes, who is 65 and often treats older adults as a general surgeon.
Carpenter, dean of the Oakland University William Beaumont School of Medicine, said his school is also encouraging students to look at primary care.
He said medicine doesn’t “do a great job” of supporting geriatricians and argued that there needs to be more incentives to go into geriatrics and primary care. One such incentive would be forgiving their student debt. The average student graduating from medical school has around $200,000 in debt, Carpenter said.
“We do not do a great job of rewarding those specialists,” he said of geriatricians, “because I think they are incredibly important to helping us take care of our aging population, but I don’t think they get the recognition and … the return on their investment that other specialties do.”
Michigan had 7,244 primary care physicians in 2023, but it needed 7,699, according to projections by the Robert Graham Center. The center says it projected the workforce necessary to maintain “current primary care utilization rates,” accounting for increased demand because of aging, population growth and an increasingly insured population due to the Affordable Care Act. The projections were developed in 2010.
‘Advanced practice’ providers fill the gap
Carey, president of William Beaumont University Hospital, said that as doctors in the baby boomer generation move into retirement age, the care model “is going to have to adapt.” He said advanced practice providers ― physician assistants and nurse practitioners ― will likely provide a higher percentage of the care than they do currently.
“And having more of them trained in the geriatric, palliative care, chronic care areas will be very important,” he said.
Michigan had 14,972 nurse practitioners in 2024, including 4,937 in Metro Detroit, according to the Michigan Professional Nurse Development program. A small percentage of these are adult-gerontology nurse practitioners, which means they are certified to care for patients 13 years and older and have received specialized education to care for the “unique needs” of patients 65 years and older, said Patrick Crane, an assistant professor and nurse practitioner at Michigan State University.
Crane said family nurse practitioners, who make up nearly 69% of nurse practitioners nationally, are also certified to care for older adults, but they see patients of other ages as well.
Naila Russell, legislative committee chair for the Michigan Council of Nurse Practitioners, said nurse practitioners can be someone’s primary care provider in Michigan. She said these practitioners are typically told that they listen well and they take a lot of time with their patients.
“And certainly with the aging population, that can be of value, right?” she said.
Finkel, Henry Ford Health’s chief primary health officer, said the system hired about 20 additional advanced practice providers to staff its primary care practices in 2024 and 2025.
He said advanced practice providers work in Henry Ford’s emergency rooms, operating rooms, and doctors’ offices.
“It’s really a critical part of the ability for us to be able to meet the demand of our growing and aging population,” he said.
asnabes@detroitnews.com
This article originally appeared on The Detroit News: As Metro Detroit greys, health systems will need more primary care providers
Reporting by Anne Snabes, The Detroit News / The Detroit News
USA TODAY Network via Reuters Connect